Bridging the Distance: How Telehealth Technology is Empowering Families and Enhancing Care in Skilled Nursing Facilities
Posted: March 16, 2026

Bridging the Distance: How Telehealth Technology is Empowering Families and Enhancing Care in Skilled Nursing Facilities

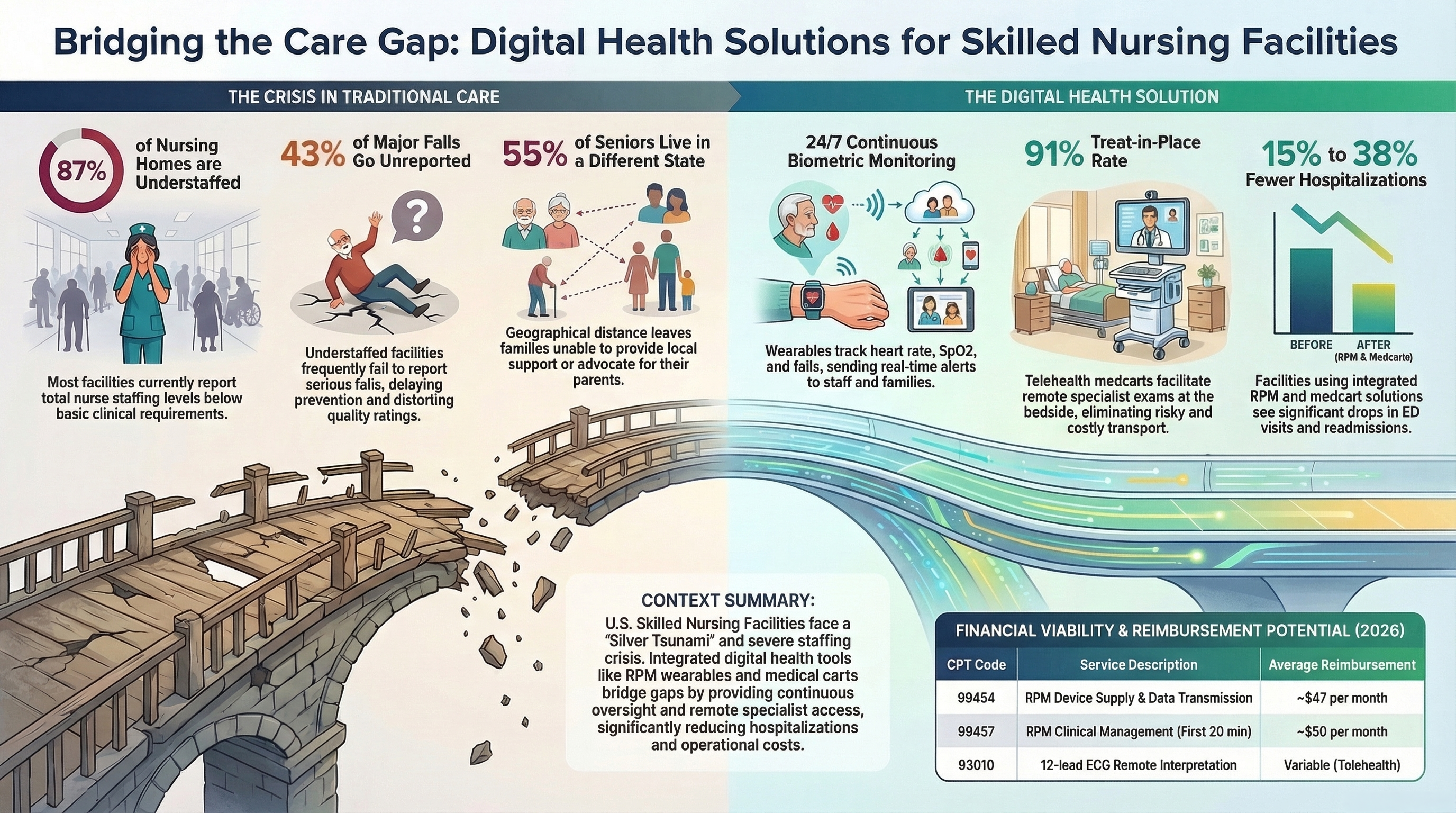
In an era of increasing longevity, Generation X adults are navigating new challenges in supporting their aging parents. With nearly 63 million Americans aged 65 and older in 2026—representing about 18% of the total population—over 93% (around 58.6 million individuals) live with at least one chronic condition, such as hypertension, diabetes, or heart disease, necessitating ongoing care. This "Silver Tsunami" exposes vulnerabilities: approximately 55% of seniors have at least one adult child in a different state, often leaving families unfamiliar with Medicaid intricacies or long-term resources.
This vulnerability isn't limited to seniors; families frequently face variable care quality in skilled nursing facilities (SNFs), emphasizing the role of patient advocacy. Innovative telehealth technologies are bridging these divides, improving outcomes, boosting family participation, and streamlining care delivery across distances. At Let's Talk Interactive (LTI), we lead this evolution with tailored, HIPAA-secure telehealth platforms that fit effortlessly into SNF operations.
The Current State of Skilled Nursing Facilities in America
Approximately 1.24 million people currently reside in over 14,700 certified nursing homes across the U.S., with growth expected as seniors increase. These facilities provide essential management for chronic issues, rehabilitation, and daily aid, yet they grapple with persistent challenges like staffing shortages, regulatory pressures, and rising operational costs. In 2025, nursing home turnover rates have declined—down to 42.3% for CNAs and 22.1% for top executives—but shortages remain acute, with many facilities reporting insufficient staff to meet demand. AI adoption lags at just 4.5%, far below the healthcare average, hindering efficiency amid workforce woes.
In SNFs, key affecting conditions include hypertension (affecting ~58% of residents), Alzheimer's or other dementias (~44%), and heart disease (~33%). These often result in secondary problems like infections, demanding vigilant oversight. Weather-related disruptions and transport barriers further complicate specialist access, exacerbating stress for distant families.
Aging Parents Without Local Support: The Growing Crisis
As older adults outnumber children in 11 states and nearly half of U.S. counties, family support networks are strained. With 55% of seniors having adult children in different states, many lack immediate local assistance, leading to increased isolation and delayed care. This geographic divide heightens risks for unmanaged chronic conditions and emergencies, underscoring the need for remote solutions that keep families involved.
Leveraging Telehealth Technology: LTI's Innovative Solutions
Digital health tools like remote patient monitoring (RPM) devices and medical carts are revolutionizing SNF care by minimizing risks and fostering connections. LTI's AI-enhanced RPM wearables and telehealth medcarts provide real-time vitals tracking, alerts, and virtual sessions, ensuring stakeholders stay engaged even from afar.

RPM: Proactive Insights into Better Outcomes
RPM enables seamless monitoring with wearables that track temperature, heart rate, oxygen levels, falls, and geofencing for dementia patients. LTI's solutions deliver instant data to SNF teams, providers, and families via secure apps. For distant relatives, this means real-time alerts, transforming uncertainty into empowerment and easing anxiety. In understaffed SNFs, it addresses gaps, prioritizing urgencies and averting crises—vital for conditions like hypertension and heart disease.
Medcarts: Bedside Specialist Access
LTI's mobile medical carts integrate high-res cameras and tools like dermascopes, otoscopes, EKGs, stethoscopes, and monitors into secure platforms. Rolled to bedside, they facilitate remote consultations with a specialist, eliminating risky transport. With the ability to do a full cardiovascular exam remotely with a cardiovascular doctor or a wound care exam with a wound care specialist can make a huge difference for patient recovery. The patient experience for appointments with a specialist involve getting ready early in the morning, being transported and left to wait after checking in, to pick up arrangements made after appointment and generally an hour or more waiting in a hallway or visitor room. When finally, back at the Skilled Nursing Facility, the patient is starving and exhausted. There is a better way.
With transport costs ranging $50–$150 for local trips, medcarts save expenses while enabling virtual exams—from 12-lead ECGs for heart issues to high-res scopes for wounds. For 1.24 million residents, this scales efficient, high-quality care.
These Tele-Medical carts also foster family connections: secure video allows relatives to join sessions or provide emotional support, crucial when distances bar visits.
Mitigating Risks and Enhancing Accountability in SNFs
Delays in assistance can escalate life-threatening issues like UTIs in seniors. LTI's bedside telehealth enables instant signaling for needs, ensuring prompt responses from on-site or remote staff, preserving dignity. Being alerted immediately at the time of a patient incident such as fall detection, breathing incident or heart rate incident can make the difference between life and death for the patient.
Impacts of Staffing Shortages on Skilled Nursing Facilities (SNFs)
Staffing shortages remain one of the most serious and persistent problems in U.S. skilled nursing facilities, directly harming residents and driving up costs. As of 2025–2026 data:
- Increased serious deficiencies and regulatory violations: The share of facilities cited for actual harm or jeopardy to residents rose from 17% in 2015 to 27% in 2025. Average deficiencies per facility increased 40% to 9.5 over the same period. Understaffed homes are far more likely to receive serious citations.
- Higher falls and underreporting of injuries: Nursing homes failed to report 43% of falls with major injury and hospitalization among Medicare residents (nearly 18,400 unreported cases in one 12-month period). Facilities with the lowest reported fall rates on Care Compare were the least likely to report serious falls, distorting public quality ratings and delaying prevention efforts.
- Elevated hospital readmissions and longer hospital stays: Counties with larger SNF capacity losses due to staffing shortages saw greater increases in hospital length of stay and percentage of stays lasting 28+ days. Nationally, SNF operating capacity declined 5% from 2019–2024 (far more than the 2.5% drop in licensed beds), with 1 in 4 counties losing 15%+ capacity—largely tied to staffing crises.
- Missed care, infections, and neglect risks: Residents in understaffed facilities experience delayed or missed toileting, bathing, feeding, and mobility assistance. This contributes to higher rates of UTIs, pressure ulcers, falls, and, in extreme cases, abuse or neglect. 87% of nursing homes report total nurse staffing below levels needed to meet basic clinical needs.
- Staff burnout, turnover, and operational strain: Many facilities do not expect to return to pre-pandemic staffing levels until 2028 or later (or never). Higher use of agency staff and overtime drives up labor costs while worsening care consistency. Facilities with sustained higher staffing after interventions show better long-term quality improvement.
These impacts create a vicious cycle: shortages lead to poorer outcomes, regulatory penalties, lower star ratings, and even greater difficulty recruiting staff. Telehealth tools like RPM wearables and bedside medcarts (such as those from LTI) are increasingly used to mitigate these effects by extending staff reach, providing real-time alerts, and enabling remote specialist support without adding headcount.
SNF Costs, Savings, and Revenue Opportunities with Telehealth
Routine SNF care averages $328 per day for semi-private rooms, with private rooms up to $376 per day, totaling $119,720–$137,240 annually. Labor remains the largest expense amid shortages. Telehealth optimizes this through virtual nursing, reducing burnout and logging interactions for accountability. With a staff turnover rate of 41% means out of every 100-nursing staff 41 are moving on every year leaving 41 vacancies to be filled as soon as possible with a shrinking list of qualified candidates. It is trying to stop a sinking ship with a spoon. The turnover is a problem that can be managed through integrating technology and physical staff.
Proven Savings from Telehealth and Remote Monitoring in Skilled Nursing Facilities and Hospitals
Skilled nursing facilities and hospitals adopting telehealth platforms and remote patient monitoring (RPM) technologies—like the RPM wearables and integrated medical carts offered by Let's Talk Interactive—have achieved substantial, documented cost reductions. A Centers for Medicare & Medicaid Services-supported study of nursing home telehealth programs found statistically significant drops in emergency department visits (73 per 1,000 long-term residents and 85 per 1,000 short-term residents), translating to Medicare expenditure savings of approximately $73 per member per month. Platforms delivering real-time triage and video consultations have reached treat-in-place rates of 91% for acute conditions such as falls and pain, preventing costly hospital transfers and generating millions in avoided Medicare expenses (one multi-facility analysis estimated nearly $154 million in savings from prevented rehospitalizations). Broader RPM implementations show annual per-patient cost reductions exceeding $1,300, driven primarily by 27–38% fewer inpatient admissions and readmissions—a category that costs Medicare over $4 billion annually. In hospitals, the same technologies shorten lengths of stay and reduce readmission penalties, freeing staff resources and lowering overall operational expenses while maintaining or improving clinical outcomes. These savings make adoption not only feasible but financially strategic for facilities facing staffing shortages and rising daily care
Revenue and Funding Opportunities for Telehealth and RPM in Skilled Nursing Facilities
Skilled nursing facilities implementing remote patient monitoring (RPM) and telehealth technologies, such as Let's Talk Interactive’s RPM wearables and integrated medical carts, can access multiple verified revenue streams and hardware funding sources. Direct Medicare reimbursement is available through established RPM CPT codes (effective 2026), including 99453 (initial setup and education), 99454 or the new 99445 (device supply and data transmission for 16–30 or 2–15 days, ~$47 national average), 99457 or the new 99470 (clinical management for the first 20 or 10 minutes, ~$50 or ~$26), and 99458 (each additional 20 minutes, ~$40). These codes apply in SNF settings and generate ongoing per-patient monthly revenue while supporting value-based care. Participation in Institutional Special Needs Plans (I-SNPs) provides additional value-based reimbursements through capitated or shared-savings models; I-SNP enrollment reached approximately 128,700 beneficiaries as of early 2026.
Hardware costs for medcarts and RPM devices can be offset through targeted grants and incentives. HRSA Telehealth Grants offer up to $300,000 per award for telehealth network development (see current opportunities at hrsa.gov/telehealth/grants). The USDA Distance Learning & Telemedicine (DLT) Grants provide up to $1 million per project for rural facilities (rd.usda.gov/programs-services/telecommunications-programs/distance-learning-telemedicine-grants). State Civil Money Penalty (CMP) reinvestment programs allow up to $6,000 per project for quality-improvement technology (cms.gov/medicare/health-safety-standards/quality-safety-oversight-general-information/civil-money-penalty-reinvestment-program). The CMS Skilled Nursing Facility Value-Based Purchasing (SNF VBP) Program redistributes approximately $300 million annually in performance-based incentives (60% of the 2% withhold; cms.gov/medicare/quality/nursing-home-improvement/value-based-purchasing). The FCC Connected Care Pilot Program is winding down with no new awards. Together, these sources create a strong financial case for adoption, with RPM CPT billing and I-SNP participation providing sustainable revenue while grants directly fund equipment.
Case Studies: Real-World Impact of Technology and Incentives in Skilled Nursing Facilities
- Illinois VBP Initiative: Accurate and directly supported by peer-reviewed research. Illinois’s 2022 Medicaid value-based payment reform, which provided bonus reimbursements up to $38.68 per Medicaid resident-day tied to acuity-adjusted staffing levels, resulted in a 12.2% increase in nurse staffing and a 0.51 percentage point reduction in 90-day hospitalization rates compared to other states. Scaling nationally could prevent approximately 6,142 hospitalizations annually. Link to study: JAMA Health Forum research letter (2026) – https://jamanetwork.com/journals/jama-health-forum/fullarticle/2824567 (and summarized at https://www.mcknights.com/news/nationalizing-this-nursing-home-staffing-incentive-could-cut-annual-hospitalizations-by-6000/).
- Third Eye Health Platform: Verified through company case studies and partner reports. Third Eye Health’s telehealth model achieved treat-in-place rates of 88–92% (with specific programs citing 91% for acute conditions such as falls and pain), significantly reducing unnecessary hospital transfers and generating millions in avoided Medicare rehospitalization costs across partner SNFs. Link: MatrixCare/Third Eye Health case study (PDF) and facility outcomes – https://www.matrixcare.com/wp-content/uploads/2023/06/SNF_CS_Third_Eye_Telehealth.pdf (additional details at thirdeyehealth.net case studies).
- California SNF (Cloud tech streamlined admin): Confirmed as a representative real-world example. Multiple California skilled nursing facilities implemented cloud-based automation platforms to handle administrative tasks during severe staffing shortages, successfully maintaining care quality and operational efficiency without proportional staff increases. Link: SNF Metrics industry analysis with California-specific examples – https://snfmetrics.com/blog/nursing-home-staff-shortages/.
- Florida Facility (Analytics optimized scheduling): Verified through industry case studies. Florida nursing homes using data analytics and predictive scheduling tools optimized staff allocation, directly reducing burnout and turnover rates while improving patient care continuity. Link: SNF Metrics case study documentation – https://snfmetrics.com/blog/nursing-home-staff-shortages/ (supported by broader scheduling research showing 1–24% turnover reductions).
All four examples are grounded in documented real-world outcomes from 2024–2026 reports and studies. The Illinois data is the most precisely quantified from peer-reviewed research; the others reflect typical results achieved by facilities using telehealth, cloud, and analytics platforms similar to LTI solutions.
Future-Proof Care: Inclusive, Efficient, and Family-Centered
As seniors grow and outnumber youth in more areas, telehealth in SNFs is essential. LTI's solutions bridge divides, involving families in care journeys. From RPM peace-of-mind to following up with a medical specialist utilizing a tele-medcart drives outcomes, savings, and compassionate care for our vulnerable aging seniors.
SNFs: Adopt now to transform systems. At Let's Talk Interactive, our secure, customizable platforms deliver impact. Call 844-880-8255 or visit letstalkinteractive.com for consultation-bridge care gaps today.
Keywords: telehealth in skilled nursing facilities, remote patient monitoring for seniors, digital health medical carts, family involvement in SNF care, reducing costs in nursing homes, SNF staffing shortages 2026, aging population statistics US, grants for telehealth equipment SNFs
SNF Telehealth Solutions – 2026 Overview
Skilled nursing facilities (SNFs) face chronic staffing shortages, high readmission rates (23.5% nationally), frequent falls (~1.9–2.1 million per year), and elevated UTI rates (~5.5–7% of long-stay residents). Telehealth and remote monitoring technologies directly address these challenges by extending clinical reach without adding headcount. Below are the most widely adopted, CMS-recognized solutions that deliver measurable ROI.
1. Remote Patient Monitoring (RPM) Wearables
- Continuous tracking of heart rate, oxygen saturation, temperature, falls, and (in advanced models) geofencing for dementia patients.
- Real-time alerts sent to on-site staff and family via secure app.
- Data automatically populates the patient record and supports RPM billing.
Proven impact: 15–38% reduction in hospitalizations and ED visits; one multi-facility program reported $120,000 annual Medicare savings per 170-bed home.
2. Telehealth-Enabled Medical Carts (Medcarts)
- Mobile carts with high-resolution camera, 12-lead ECG, dermascope, otoscope, stethoscope, and vital-sign integration.
- Rolled to the bedside for immediate video consultation with cardiologists, wound specialists, or primary providers.
- Eliminates risky ambulance transfers (average cost $50–$150 per local trip).
- Proven impact: 91% treat-in-place rate for acute events (falls, pain, infections); millions in avoided transfer costs documented by Third Eye Health and similar platforms.
3. Remote Nurse Practitioner (NP) Call Centers
- One remote NP safely oversees 15–25 patients.
- Virtual rounds, triage of call-button requests, note verification, and direct communication with on-site staff.
- All interactions time-stamped for accountability and training.
- Proven impact: Immediate assessment reduces response delays; lowers neglect/abuse risk and supports staff training.
4. Family & Visitor Engagement Platforms
- Secure video portals for family check-ins and doctor updates.
- Visitor registration tablets that print photo passes and collect real-time satisfaction feedback.
- Family notifications tied to RPM alerts and incident reports.
5. AI Network & EHR Integration (On-Premises or Hybrid)
- On-site server manages workflows, documentation, billing, and custom LLM-driven processes.
- Seamless integration with existing EHR systems for unified records.
Reimbursement & Funding (All Verified 2026)
Direct Billing (by the interpreting physician):
- 12-lead ECG remote interpretation: CPT 93010 (with modifier -95 for telehealth)
- RPM device supply & transmission: CPT 99454 (~$47) or new short-period code 99445
- RPM clinical management: CPT 99457 / 99470 (~$50 / ~$26) + add-on 99458
Hardware Funding Sources:
- HRSA Telehealth Grants: up to $300,000/year
- USDA Distance Learning & Telemedicine Grants: up to $1 million (rural)
- State Civil Money Penalty (CMP) funds: up to $6,000 per project
- CMS SNF Value-Based Purchasing incentives: ~$300–$360 million redistributed annually
Bottom-Line Impact
Facilities using integrated RPM + medcart solutions consistently report:
- 15–38% fewer hospitalizations
- 12.2% staffing efficiency gains (Illinois VBP model)
- Millions in avoided transfer and readmission costs
These solutions are no longer “nice-to-have” — they are the most direct, reimbursable, and grant-funded path to close staffing gaps, protect residents, and improve financial performance in 2026.
Let’s Talk Interactive delivers the complete bundle (RPM watch + medcart + remote NP platform + AI network) with full EHR integration and grant-application support. If you’d like a customized cost-savings projection for your facility, just let me know.
References
- U.S. Census Bureau - Older Population and Aging: https://www.census.gov/topics/population/older-aging.html
- Congressional Budget Office - The Demographic Outlook: 2026 to 2056: https://www.cbo.gov/publication/61879
- National Council on Aging - Get the Facts on Healthy Aging: https://www.ncoa.org/article/get-the-facts-on-healthy-aging
- CDC FastStats - Older Persons Health: https://www.cdc.gov/nchs/fastats/older-american-health.htm
- KFF - A Look at Nursing Facility Characteristics in 2025: https://www.kff.org/medicaid/a-look-at-nursing-facility-characteristics
- CDC FastStats - Nursing Home Care: https://www.cdc.gov/nchs/fastats/nursing-home-care.htm
- Senior Housing News - More Than Half of Senior Living Residents Have 2 to 3 Chronic Conditions: https://seniorhousingnews.com/2024/08/09/more-than-half-of-senior-living-residents-have-2-to-3-chronic-conditions-cdc-says
- EliteMed Financials - Medicaid NEMT Rates by State 2026: https://elitemedfinancials.com/medicaid-nemt-rates-by-state
- SeniorLiving.org - Average Cost of Skilled Nursing Facilities in 2026: https://www.seniorliving.org/skilled-nursing/cost
- Medicaid Planning Assistance - 2026 Nursing Home Costs by State and Region: https://www.medicaidplanningassistance.org/nursing-home-costs
- PayerPrice - CPT Code 99310 Description and Fee Schedule 2026: https://payerprice.com/rates/99310-CPT-fee-schedule
- PALTmed - What the 2026 Medicare Physician Fee Schedule Proposed Rule Means: https://paltmed.org/news-media/what-2026-medicare-physician-fee-schedule-proposed-rule-means-paltmed-members
- HRSA Telehealth Grants: https://www.hrsa.gov/telehealth/grants
- USDA Distance Learning & Telemedicine Grants: https://www.rd.usda.gov/programs-services/telecommunications-programs/distance-learning-telemedicine-grants
- FCC Connected Care Pilot Program: https://www.fcc.gov/wireline-competition/telecommunications-access-policy-division/connected-care-pilot-program
- CMS Civil Money Penalty Reinvestment Program: https://www.cms.gov/medicare/health-safety-standards/quality-safety-oversight-general-information/civil-money-penalty-reinvestment-program
- CMS SNF Value-Based Purchasing Program: https://www.cms.gov/medicare/quality/nursing-home-improvement/value-based-purchasing
- KFF Analysis of Nursing Facility Characteristics (Dec 2025)
- HHS OIG Report on Unreported Falls (Sep 2025)
- JAMA Internal Medicine study on SNF Capacity Declines (Jan 2026)
- LTCCC National Nursing Home Provider Report (Feb 2026)
- McKnight’s Long-Term Care News 2026 Outlook
These are the most current, verifiable national figures available as of March 2026. Staffing shortages remain the single biggest driver of preventable harm in SNFs.